ATRIAL FIBRILLATION CARDIOVERSION
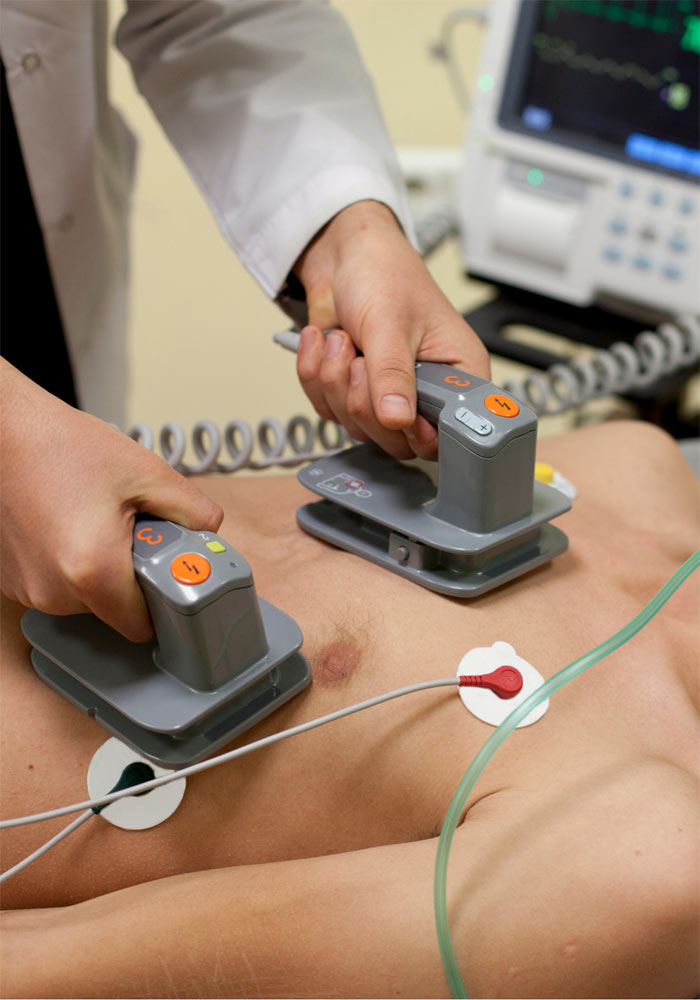
ARRHYTHMIA CARDIOVERSION
In some cases in which the heart rhythm is “irregular” (e.g. atrial fibrillation or atrial flutter) the physician after taking into account the patient’s complete medical history, available treatment options may suggest the conduction of cardioversion in the context of a “rhythm control” strategy.
Particularly speaking of atrial fibrillation or atrial flutter this is a procedure that may be conducted in the acute phase (within 48 hours after a “new” arrhythmia) or electively (in this case treatment with anticoagulants at an appropriate dose for at least 21 days must precede). Additionally, a transesophageal echocardiography may be needed.
Cardioversion, ie the “reset” of the patient’s heart rhtyhm from an arrhythmia to the normal sinus rhythm can be done either pharmacologically or electrically (via administration of -synchronized- electrical defibrillation).
Pharmaceutical cardioversion is usually performed in a hospital setting either due to the need for intravenous administration of the drug (eg amiodarone) or for management and treatment of potential adverse drug reactions, especially if the patient is administered for the first time (e.g. propafenone). Pharmaceutical cardioversion usually needs several hours to restore the heart rhythm.
Electric cardioversion is always performed in a hospital setting. The patient is administered mild sedation (anesthesia) so that the electric shock is not to be perceived. Heart rythm restoration is immediate. In most of the cases the patient returns to daily routine the same afternoon. However, in some cases a 24-hour follow-up may be required.
The main risk in the process of restoring your heart rhythm is to cause an ischemic stroke – this is why there are very specific “rules” in relation to the onset of the arrhythmia and the administration of anticoagulants. If these are taken care of, then the risk is minimized. Other side effects are uncommon and transient (headache, dizziness, local pain at the site of the shock).
