PERCUTANEOUS CORONARY INTERVENTION
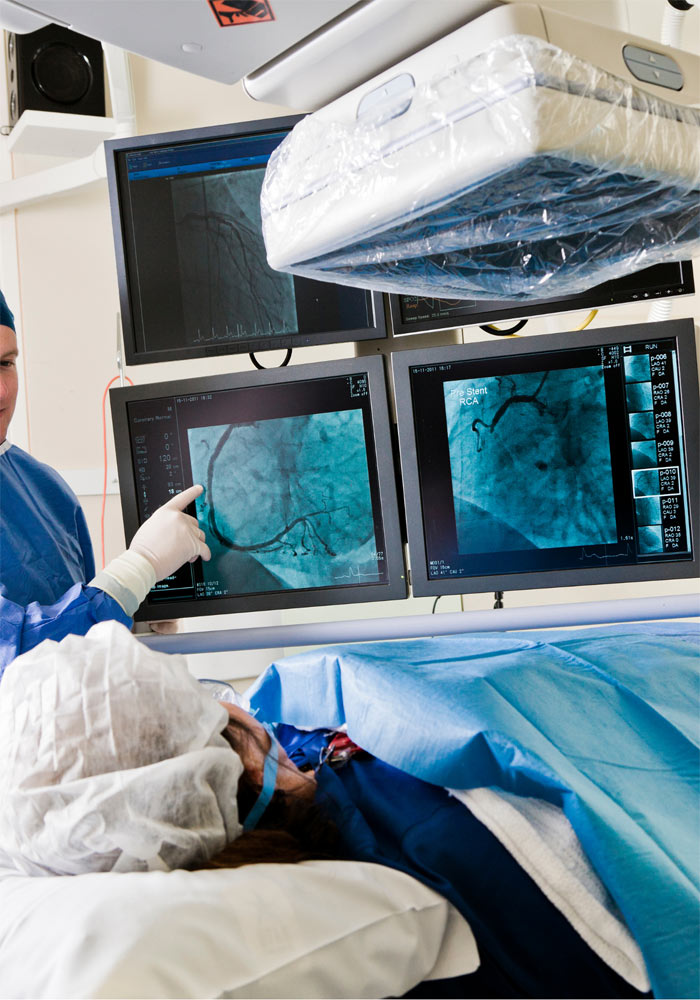
CORONARY ARTERY ANGIOPLASTY – STENT IMPLANTATION
Percutaneous coronary interventions are performed to “restore” a narrowing or obstruction of the coronary artery lumen. Coronary arteries are those vessels that carry oxygenated blood to the myocardium. Historically, these operations involved only dilating (inflating) a special bag (balloon) into the lumen of the vessel.
From the 1970s when the method was introduced until today the technical means used have shown rapid growth. Now, in the vast majority of cases, a skeleton (scaffold) of special alloys called a stent (coronary stent prosthesis) is implanted. Newer generation stents consist of a thin scaffold and carry special drugs that prevent restenosis (Drug Eluting Stents – DES) in contrast to the older ones (Bare Metal Stents – BMS). Patients receiving a stent should be treated with antiplatelet drugs for prolonged periods. The exact medication scheme (drug combination; duration) is chosen upon the balance between the estimated risk of ischemia versus the risk of bleeding events.
When is PCI indicated?
In the case of acute myocardial infarction PCI is a life-saving intervention conducted in urgent basis (literally called primary PCI). Both globally and in Greece, the introduction of primary PCI programs has significantly reduced death from acute myocardial infarction and the percentage of patients who develop heart failure after acute myocardial infarction.
PCI is also performed on a electively when the combination of findings from coronary angiography and / or functional techniques indicate that a critical section of the myocardium is at risk for ischemia (due to significant coronary artery disease) or as a last resort to treat angina.
In cases of severe coronary artery disease, especially in diabetic patients, or if anatomical features of the coronary network suggest that PCI will be complex then it is recommended that the patient undergo coronary artery bypass grafting (coronary artery by-pass grafting;CABG) as the risk / benefit balance compared to the two methods leans in favor of surgery.
How is PCI conducted?
PCI is performed in a specially organized clinic called catheterization laboratory which is properly equipped and staffed with adequately trained personnel. It is conducted under local anesthesia in the vast majority of the cases. Coronary angiography always precedes (see related article). Compared to coronary angiography, the only difference the patient perceives is the length of the procedure.
Risks
Potential complications of PCI are similar to those of coronary angiography, but there is an increased absolute risk since advancement and manipulation of special equipement (e.g. wires, catheters, balloons, stents) within the coronary arteries is conducted. Minor complications usually involve the vascular access points (material entry point) and the contrast agent (allergic reactions, deterioration of renal function – usually reversible). Significant complications include stroke, myocardial infarction or even death (less than 1% overall in elective cases).
